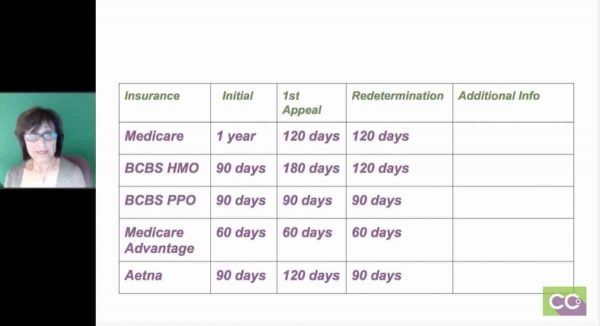
What if Medicare is the primary payer and they processed the claim after the 365 days expired? Providers have an additional 120 days from a Medicare payment or denial and must include the Medicare EOB date on the claim. What is the 365-day rule? Claims with commercial insurance/TPL must be received within 365 days with no additional extension. Providers must keep the EOB and supporting documentation on file. Providers must include the Medicare or TPL EOB date on the claim. 
Do I need to continue attaching the Explanation of Benefits (EOB) to electronic claims? Providers who receive payment from Medicare or other insurance/Third Party Liability (TPL) no longer need to attach the EOB to the electronic claim. The Delayed Notification of Eligibility form can no longer be used, as providers must submit within 365 days. If the timely filing period expires because the provider is not aware that the member is Health First Colorado eligible, the fiscal agent is not authorized to override timely filing. It is not effective to rely solely on billing statements, collection notices, or collection agencies as the only means of obtaining eligibility and billing information. Verifying eligibility through the Provider Web Portal.Contacting the member by phone or by mail. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
